Expert: America's 'legacy of racism' led to a broken drug treatment system
This post has been updated.
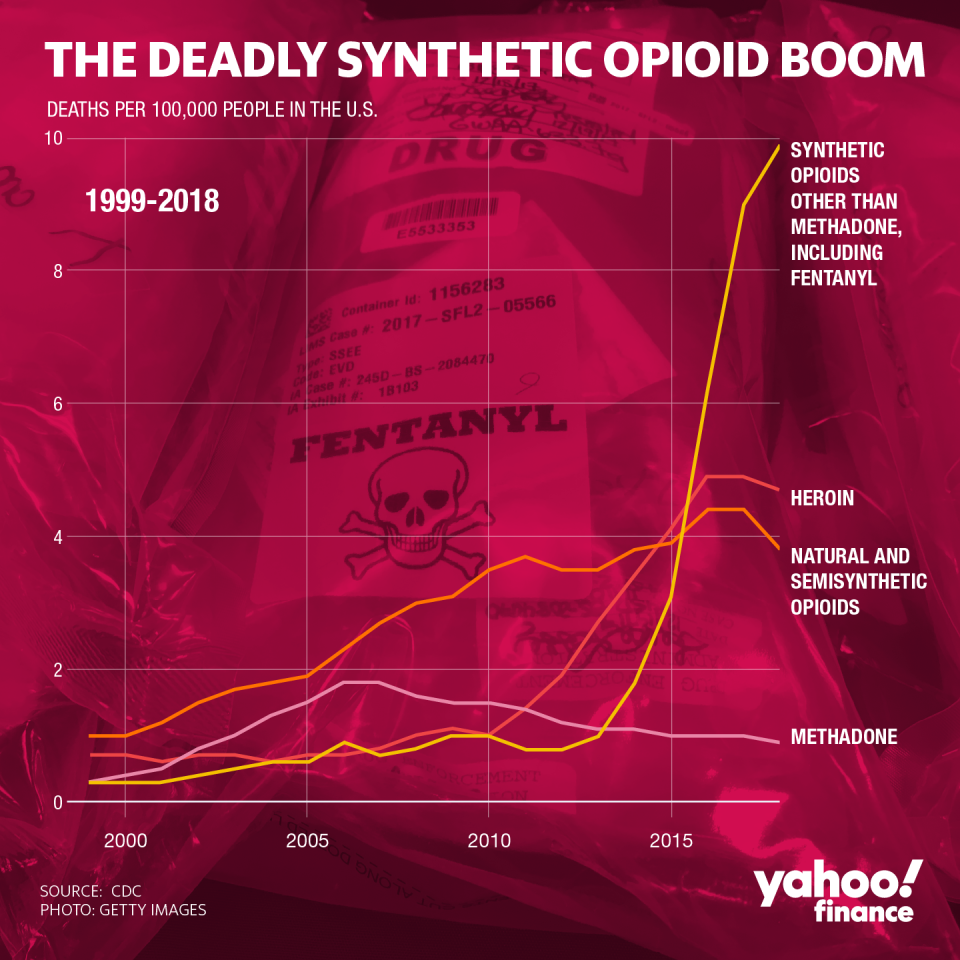
As the U.S. continues dealing with the opioid crisis, some experts argue that the American drug treatment system must reckon with its ingrained prejudices before properly tackling the problem.
“It’s the legacy of slavery, it’s the legacy of racism, it’s the segregation,” Tracie Gardner, vice president for policy advocacy at the Legal Action Center in New York, told Yahoo Finance. “And the idea that people, because of their skin color, are somehow less or different.”
Dr. Allison Lynch, director of addiction medicine at the University of Iowa, noted that “racism has been a major problem in American culture since the beginning, and so it has influenced everything in our society. There’s definitely very easy-to-identify examples of how racism has impacted substance use treatment.”
Lynch added that now that “there’s more white people who have drug addiction, we’re getting more money and more attention paid to drug addiction treatment. Before it was often viewed as a problem in urban communities, which is group-speak for minority populations. I can’t think of anything in our country that isn’t influenced by our culture of racism, and substance use treatment definitely has been influenced by that, absolutely. Today, at this minute, our system is influenced by racism.”
Lynch, Gardner, and other experts detailed how institutional racism — as it relates to lack of access to treatment, stigmas related to mental health, flawed hospital procedures, and insurance industry practices — can help explain America's struggle with combatting the evolving opioid crisis.
“The addiction treatment system, it’s not even that it’s broken — it never worked, because it was based all along on ideas of the people who would be using,” Gardner said. “And it was people we don’t care about, people who deserve to die, people who don’t deserve to have good health care, people who deserve to feel pain.”
‘She looked at me with these pleading eyes’
A 2018 study that found white Americans were twice as likely to be prescribed an opioid than black Americans due to racial stereotyping by doctors, who tended to worry that their black patients would become addicted to the medication.
That meant that fewer black patients became addicted: separate study from the journal Epidemiology that found an estimated 14,000 more black Americans would have died from opioid overdose if they had been prescribed opioids at the same rate as white Americans.
Nevertheless, the system’s apparent bias is generally a negative for black Americans: A study from the University of Michigan found that white populations were nearly 35 times as likely to receive treatment for opioid addiction than black Americans, even though there are similar rates of opioid addiction among different racial backgrounds.
The treatment is buprenorphine, one of two approved medications for treating opioid addiction (the other is methadone), and physicians have to receive certification to prescribe either of these medications.
Lynch explained that the lack of access to buprenorphine and methadone creates a barrier that does not exist with other drugs (including prescribing opioids in the first place).
“I had a patient one time, we were calling all over to find a pharmacy that had the formulation and dose that she needed, that would take care of it with insurance,” she said. “She looked at me with these pleading eyes and said: ‘It would be so much easier for me just to go down to the emergency room and tell him I have a migraine, and I need some Percocet.’”
“And she’s right,” Lynch added. “It’s crazy ... insulin, Coumadin or warfarin, a blood thinner that people are on after they’ve had a stroke. These are dangerous medicines, too, and people can die from them, and there’s no special certification to prescribe them. That’s just crazy.”

‘Ignored by the health care system’
Another issue raised by several drug policy experts, including Gardner, is that those with addiction issues are treated like they are criminals rather than individuals suffering from a disease.
“It’s not an accident that there are so many people who are in jails and prisons who have mental health and addiction issues,” Gardner said. “I contend that if they had been treated further upstream, they wouldn’t be in jail. At the point of somebody getting arrested is usually when they’re their sickest. It’s either after a run, they haven’t taken their medications, they are very sick. We have been asking the criminal justice system to treat people who have come to rest in the criminal justice system when they’ve been ignored by the health care system.”
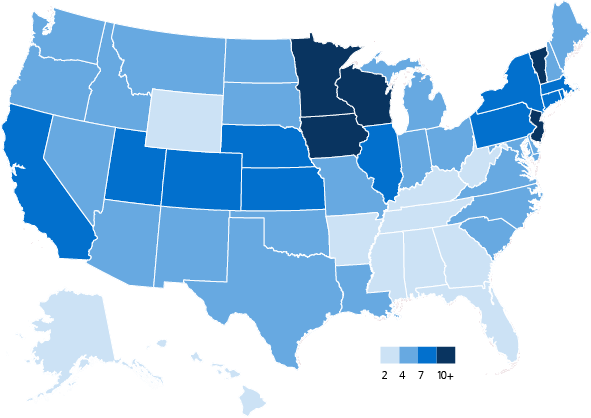
According to the National Institute on Drug Abuse, approximately 65% of those incarcerated in the U.S. has some kind of substance use disorder. And a study from the Addiction Science & Clinical Practice journal found that less than 20% of those in prison who have a substance use disorder have received some kind of formal treatment. These low figures can lead to developing substance addiction once released from prison and lead to re-incarceration. And there is a racial context: Black Americans historically outnumber White Americans in U.S. prisons.
“The public officials need to be hand-in-hand with law enforcement officers,” Cristian Herrera, health policy analyst at the Organization for Economic Cooperation and Development (OECD), previously told Yahoo Finance. “The example that exists in many countries is the drug courts. The special devices in the criminal justice system where the person who is using drugs is not treated immediately as a criminal, but instead as a person who is diseased. In the end, this person can be redirected ... to the health system to receive support.”
Gardner said that the support from the health system is inadequate for many.
“There are so many examples of where the health system has kind of relinquished its responsibility or role in treating people who present ‘primarily’ with what they would call a behavioral health issue,” Gardner said. “What is happening very, very slowly now — in one part because of money, because money is everything — is the people who have behavioral health issues have worse outcomes with their health issues.”
‘So if I came in with a heart attack...’
Gardner explained that there “are so many insidious ways” that people with drug addiction are pushed away from hospitals and emergency rooms, she said.
“A person who comes in after an overdose could be stabilized with suboxone,” Gardner said. “The idea that you’re giving them suboxone so they can get high versus you’re giving them suboxone to treat their withdrawal symptoms, that’s a mindset. Are you compassionate or do you think they deserve the pain that they’re in?”

“And emergency room doctors have said things like ‘we can’t do that because we can’t provide them with treatment,’” Gardner added. “And it’s like, ‘so if I came in with a heart attack, I’ve eaten burgers all the time but I came in with chest pain, you can’t start me on a statin or whatever it is because that’s how I came into the emergency room?’ They don’t compare, right? And that’s a lot of what’s going on too — if you do the addiction and mental health issues, then when you compare it to how we address health issues, you see where it’s lacking.”
Dr. Josh Radke, an assistant professor of emergency medicine and director of medical toxicology at the University of Iowa, said this is “one of the big problems” particularly in different emergency departments.
“There’s this stigma that gets perpetuated,” he told Yahoo Finance. “Even training in the residency, that’s the language we use. That’s the language we’re taught: drug-seeking behavior. Stigmatizing language. And so, there’s definitely that aspect where people just don’t want to come in because they don’t want to deal with that stigma.”
‘We revile people who use drugs’
The insurance system also plays into the stigma when it comes to addiction.
“People who have commercial insurance think ‘I pay premiums every month, so I should be able to get full and robust coverage for the care that my family needs,’” Gardner said. “And that’s not the case with mental health and addiction, where if you haven’t read the fine print or if you haven’t even understood that you have to meet some insane deductible before you can even get a portion of the care paid for. And again, all of this, as a society we’ve accepted it because we revile people who use drugs and people who have mental health issues. We’ve just always done it. We’ve always seen it as a kind of subcategory, sub-issue, subspecialty.”

The prejudice ingrained in insurance coverage leads to doctors not truly understanding addiction care, Gardner said, because they are not incentivized to be paid less by insurance companies while dealing with more complex claims.
“The insurance companies have been allowed to pay less for that kind of care, which then affects me as a provider,” Gardner said. “Why do I want to get into this line of care where I’m paid less and I’m going to have to go through all this BS with an insurance company? And so in many cases, there’s a shortage of providers who can provide this kind of care because either they don’t have the background or they’re not incentivized to go into the business.”
Adriana is an associate editor for Yahoo Finance. Follow her on Twitter @adrianambells.
READ MORE:
The U.S. opioid crisis will cost $800 billion over last five years, study says
Pete Buttigieg's prescription drug plan eyes funding for opioid treatment
Read the latest financial and business news from Yahoo Finance
Follow Yahoo Finance on Twitter, Facebook, Instagram, Flipboard, SmartNews, LinkedIn, YouTube, and reddit.

 Yahoo Finance
Yahoo Finance 
