Supply shortages and vaccine inequality leaves Covax facing uncertain future
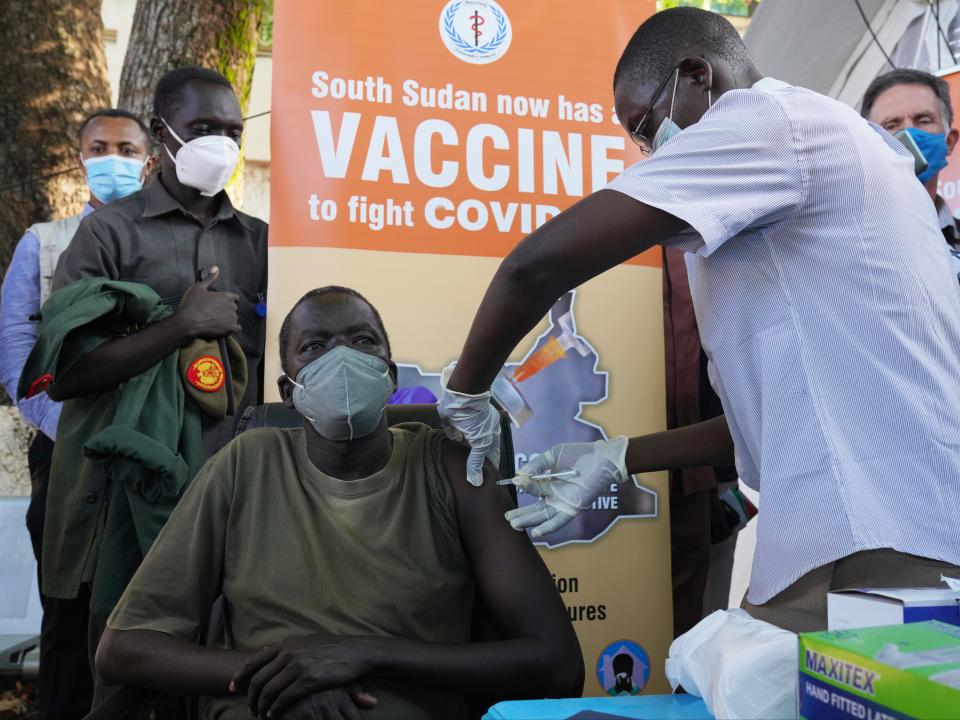
First established in the early weeks of the pandemic, when the full scale of the Covid crisis was still taking shape, the global vaccine-sharing initiative Covax faces as many challenges and hurdles today as it did back in April 2020.
The scheme, overseen by a coalition of health groups, charities and agencies, including the World Health Organisation and Gavi, has set itself the ambitious goal of delivering more than 2 billion doses to the world’s 92 poorest countries by the end of 2021.
However, amid the wave of vaccine nationalism that has swept the globe, culminating in export bans, hoarding and supply shortages, there is uncertainty over whether Covax will be able to realistically meet its objectives.
As the western world races ahead in its immunisation efforts, those in the global south face a long and agonising wait to get their hands on the life-saving Covid vaccines. The disparities between rich and poor are widening with each passing week.
From Bangladesh to Brazil and Mexico to Myanmar, countries are facing significant shortfalls in dose supplies they had expected by May, leaving healthcare workers, the elderly and the sick vulnerable to Covid-19, as lower-risk populations in the UK, US and Israel line up to receive a jab.
According to Covax documents seen by The Independent, some 237 million shots of the AstraZeneca/Oxford vaccine were due to be allocated between February and May. However, as of Wednesday, only 53.8 million shots had been delivered to 121 nations – just 22.7 per cent of its target.
The export ban placed on the Serum Institute of India (SII), the largest provider to Covax, has been blamed for the recent delays. As India battles a devastating surge in cases, doses produced by the manufacturer have been diverted away from the project to the national population.
According to one Covax source, roughly 90 million shots due to be channelled into the project by SII were held back throughout March and April, with future deliveries to set remain “uncertain in [the] coming months”.
“The attention might go on the export ban, but who thought it was a good idea to put all the eggs in one company’s basket in India,” says Kate Elder, a senior vaccines policy adviser at the Médecins Sans Frontières. “That seems worthwhile to question.”
But Covax’s challenges stretch well beyond one central manufacturer. Insiders in the project have said for months now that there simply isn’t enough production capacity across the world to guarantee a steady and accessible supply stream for the global south, which has been left behind in the rush to secure doses.
The world’s richest countries have bought one billion more doses than their citizens need, according to estimates, with vaccination coverage in these countries climbing every day.
Meanwhile, countries like Bangladesh, Pakistan and Myanmar have yet to receive a single dose through Covax. Research suggests that 9 out of 10 people in 70 low-income countries are unlikely to be vaccinated throughout 2021.
“They’re now moving to the phase where we’re talking about how do we scramble to make more manufacturing capacity,” says Elder. “I’m not so optimistic. Nothing will be too late, but shouldn’t that have been built into the original architecture in a more deliberate way.”
Short of money and factories needed to ramp up dose production, Covax has begun campaigning for countries with an excess of supplies to donate their shots to poorer countries. There has been some recent “positive steps” in this space, says Will Hall, a global policy manager at Wellcome.
Sweden, Spain and France have all said they will share their surplus doses, with the French government expecting to donate more than 10 million shots by the end of the year, The Independent has been told.
Norway and New Zealand have also chosen to return the doses they received as a result of their Covax membership, with the latter agreeing to pay for the 1.6 million shots it was due to receive.
“We need to make sure that countries with surpluses start sharing doses with those most in need now,” adds Hall. “There’s a real opportunity for countries like the UK, the US and others to show leadership in this.”
The Covax delays are having real-life consequences across the world. In Africa, at the current rates of immunisation, the continent will take a decade to vaccinate its adult population. As of 6 May, Africa’s 54 countries accounted for only 1 per cent of doses administered worldwide.
“Covax in Africa right now has stalled. We have nothing in sight until June,” says Dr Ayoade Alakija, co-chair of the Africa Union Vaccine Delivery Alliance.
Against this backdrop of stagnating vaccine rates and dwindling supplies, Dr Alakija fears the Covid crisis seen in India could soon sweep across Africa.
“What is going on in India is terrifying to behold,” she explains, saying that Africa does not have “even a hundredth” of the subcontinent’s medical capacity. “If it hits Africa like that, we are in serious trouble and we cannot afford to let that happen.”
But manufacturing and delivering vaccines is just one challenge among many. Multiple global health experts have warned of the complexities of rolling out nationwide immunisation programmes in lower-income countries, where health infrastructure and systems are woefully underfunded and poorly resourced.

“Getting vaccines to the airport in a country is only the first step. Then you need systems to make sure the vaccines get to those who need them. This is a complex logistical exercise and many countries will struggle,” says Martin McKee, a professor of European public health at the London School of Hygiene and Tropical Medicine (LSHTM).
Dr Stacey Mearns, senior technical advisor for emergency health at the International Rescue Committee (IRC), a global humanitarian aid organisation, agrees. “I think Covax is fantastic, but it solves just one piece of the equation, which is getting vaccines in countries in a more equitable manner,” she says.
Building demand, maintaining the cold chain and setting up monitoring systems are some of the additional requirements that need to be established in these countries. “If they’re not in place, it doesn’t matter if you have 100,000 vaccines,” she explains.
“Look at a context like South Sudan, where you have very poor road networks. The ability to just maintain the cold chain of those vaccines as they move from the capital to remote rural populations is enormously challenging.”
Dr Mearns is keen to stress that each country has its own particular set of challenges, and that the hurdles that present themselves in Uganda, for example, are very different from those seen in war-torn Yemen.
Having initially appeared to sidestep the worst of the pandemic, cases are now surging in Yemen, placing particular pressure on health services in the south, where treatment facilities are full and oxygen supplies are in short supply.
The country received 360,000 doses through Covax on 31 March but these shots lay idle for three weeks due to logistical issues before officials started administering them to care workers and the elderly. However, as with other low-income countries, vaccine hesitancy is high.
According to health campaigners on the ground, local communities are questioning why richer countries are donating their doses, assuming them to be defective and unsafe. “The thought pattern is understandable when the world has repeatedly let Yemen down,” says one charity worker, who asked not to be named. “Even doctors and nurses are suspicious.”
Some have argued that the open sharing of vaccine “blueprints” between manufacturers would ramp up the global production of doses and breathe new life into Covax. Earlier this week, the Biden administration took the historic step of saying it supported the WHO’s proposals to waive intellectual property rights.
One senior scientific adviser to the UK government, which has yet to throw its support behind the policy, said the move holds the potential to “stimulate” manufacturing sites in the global south and usher in “longer-lasting effects” in terms of dose production. However, in the short-term, this approach may not reap the desired rewards, the adviser said.
Professor Sarah Gilbert, the brains behind the Oxford/AstraZeneca vaccine, explains that there are multiple challenges involved in exchanging vaccine technology between companies, from maintaining safety production standards at factories to ensuring high yields are maintained.
“I’ve heard people say: ‘Give us the formula and we’ll make the vaccine in other places.’ But it’s not just the formula. That’ll be like giving someone a list of ingredients for cake and then they’ve got to work out what to do with them,” she says.
Dedicating resources, time and manpower to help inexperienced companies and factories through the process of safely manufacturing the different Covid vaccines, while ensuring a high enough amount of doses are made, could take away from the current lines of production, she adds.
Nonetheless, there is widespread acknowledgment that greater co-operation is needed in all forms to deliver the lofty goals set by Covax.
From vaccines to Covid-19 treatments, whether that’s drugs or basic oxygen supplies, the world must do more to ensure that no single country is limited in accessing these life-saving tools.
“What has been clear for a long time but has not necessarily been heeded is that everyone is in this together,” says Dr Mearns. “We’ve known this from the outset, and I hope the world is waking up to this: we’re all in a chain in this pandemic and it will not be over until it’s over everywhere.”
Read More
UK Covid-19 vaccinations: Latest figures

 Yahoo Finance
Yahoo Finance 